Off-label azathioprine - Bullous pemphigoid
Uitgangsvraag
What is the safety and efficacy of off-label treatment with azathioprine in patients with dermatological diseases?
- Bullous pemphigoid
Aanbeveling
Monotherapy
|
Weak |
There is a weak recommendation for treating bullous pemphigoid with azathioprine alone if treatment with oral corticostroids is contraindicated or has failed (very uncertain estimate for an effect of very uncertain magnitude). |
Combination therapy
|
Weak |
There is a weak recommendation for treating bullous pemphigoid with a combination of AZA and oral corticosteroids (no significant benefit of AZA). When there is a need for a corticosteroid sparing effect and a reduction of the cumulative steroid dose combination therapy may be considered (uncertain estimate for a moderate steroid sparing effect). Extra attention should be given to safety aspects when prescribing azathioprine (uncertain off-label safety). |
Overwegingen
|
Important subjets to consider |
Remarks |
|
Uncertainty in the estimates of likely benefit, and likely risk, inconvenience, and costs*
* estimates for benefit (efficacy/effectiveness) and safety are ranked by the working group as very certain, certain, uncertain or very uncertain. |
-Three randomized trials (moderate quality of evidence) have demonstrated no significant benefit of AZA in bullous pemphigoid patients already treated with oral corticosteroids. Certain estimate. -One randomized trial and one case series found a significant oral corticosteroid sparing effect. One cohort showed no significant corticosteroid sparing effect. Uncertain estimate. -One case series reported 40% well controlled disease/remission, 10% moderate response, 10% stopped due to AE and 40% died. Very uncertain effect. -Frequent side-effects: gastro-intestinal complaints, abnormal laboratory markers. Uncertainty about the off- label safety of azathioprine. -Costs may vary with the number of follow-up visits and dosage of azathioprine. |
|
Importance of the outcome that treatment prevents |
-Complete clearance of blisters -Controlled disease -Cumulative steroid dose -Death |
|
Magnitude of treatment effect* * the magnitude of treatment effect is ranked by the working group as good, moderate, low, no effect or worsening |
-No significant effect regarding to complete clearance of blisters and controlled disease compared with oral corticosteroids. No effect. -45%-50% sparing in cumulative oral corticosteroids dose. Moderate effect. -One case series 40% well controlled disease/remission, 10% moderate response, 10% stopped due to AE and 40% died. Very uncertain magnitude (worsening to good). |
|
Precision of estimate of treatment effect* * estimates are ranked by the working group as very certain, certain, uncertain or very uncertain. |
-Large confidence intervals; for example complete remission was achieved after 23.8 days treatment with azathioprine but with a standard deviation of 18.9 days. Uncertain precision. Monotherapy: very uncertain precision (see Magnitude of treatment effect). |
|
Risks associated with therapy |
-See section “general treatment considerations” and “safety”. |
|
Burdens of Therapy |
-During the first weeks of therapy laboratory monitoring at weekly intervals is necessary, afterwards every one to three months. See also section “general treatment considerations”. |
|
Risk of target event |
- 100%. |
|
Costs |
- Costs of AZA are between € 10,14 and 10,17 for 15 days 3dd 50 mg, not included are the costs for delivery, laboratory monitoring and visits to the clinic. (*www.medicijnkosten.nl). |
|
Varying Values between patients |
- |
|
Other |
- |
Onderbouwing
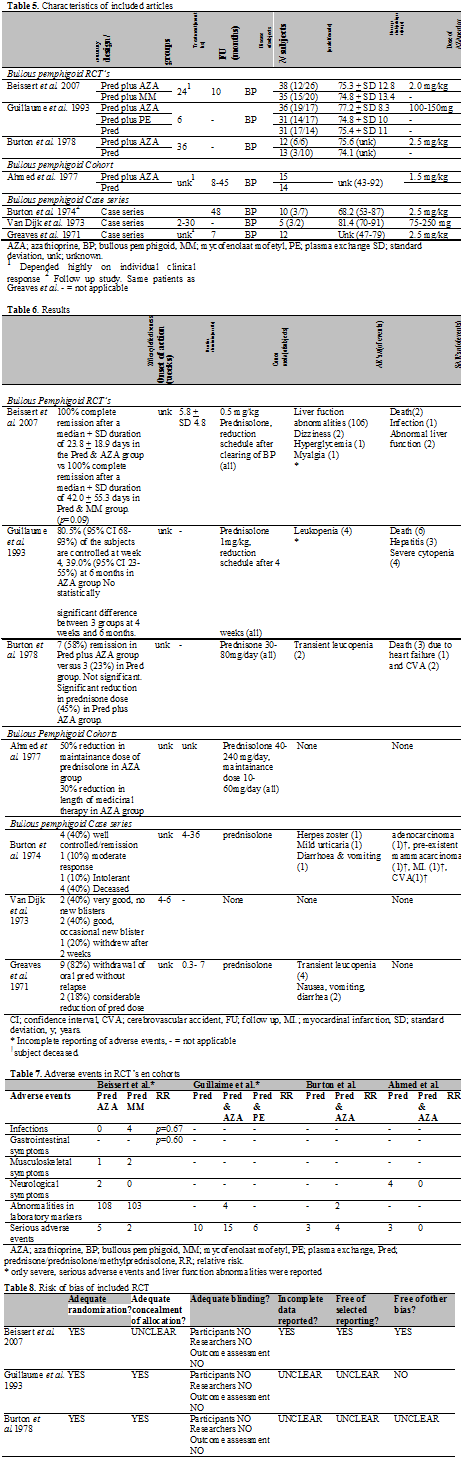
In total, 7 studies published between 1971 and 2007 were found in which patients with bullous pemphigoid (BP) were treated with AZA: 3 RCT’s, 1 cohort and 3 case series.
Efficacy/effectiveness was measured by the percentage of patients with a complete remission or controlled disease (defined as: no new blisters in the last week, mild pruritus and resolution of erythema), number of cumulative doses of concomitant oral corticosteroids, dose of oral corticosteroids at which the patient relapsed and duration of hospitalization.
Also the time to remission, duration of remission, time to relapse and number of deaths were used to assess efficacy. Laboratory markers like anti-basement membrane zone (BMZ) antibodies were also used to monitor disease severity.
Monotherapy
|
Very Low |
The only available case series considering monotherapy with AZA is of very low methodological strength with sparse data and some uncertainty about directness. The reported effect shows 40% well controlled disease/remission, 10% moderate response, 10% stopped due to AE and 40% died. |
Combination therapy
|
Moderate |
The three available RCT’s are of moderate quality due to serious limitations in study quality (also see Table 8). Although there seems to be a steroid sparing effect, there is no significant effect of azathioprine in addition to oral corticosteroids. The other evidence consisting of one cohort study and three case series shows some inconsistency with the RCT’s regarding the effectiveness. A reduction of maintenance dose of oral corticosteroids, a reduction in length of therapy and a lower dose of oral corticosteroids at which subjects will relapse was seen. The inconsistency does not decrease the level of evidence (heterogenous outcome parameters). |
RCT’s
Methodological quality
All three RCT’s employed an adequate randomization. Concealment of allocation was adequate in 2 and unclear (not described) in the study of Beissert et al. None of the trials were double blinded. Beissert et al. judge that the outcome measurement is not likely to be influenced by lack of blinding, since complete clearance of the lesions was their primary outcome and this could not be subject to interpretation of the observer. However, the cumulative dose of oral corticosteroids used during the study was also used as a primary outcome and this outcome is prone to bias . The same is true for the study of Burton et al. Guillaume et al. They defined their primary outcome as ‘controlled disease’ which could clearly be subject to interpretation of the observer.
The study by Guillaume et al. was interrupted after the interim analysis and (hence) no significantly results were found. Moreover, safety aspects were insufficiently described. In the publication of Burton et al. the methods were only briefly delineated and the methodological quality could hardly be assessed. Overall, Beissert et al. performed the most methodological sound study. An overview of the methodological quality can be seen in the risk of bias table (Table 8).
Demography
Two treatment arms were compared in the studies of Beissert et al. and Burton et al. and 3 treatment arms in Guillaume et al. AZA was never applied as monotherapy, but always in combination with oral steroids. There was no crossoverbetween the treatment arms. Duration of treatment ranged from 6 to 36 months and depended highly on individual treatment response. The dosage employed ranged from 100-150 mg and 2.0-2.5 mg/kg/day. Follow-up was carried out in one study for the duration of 10 months.
In total, 196 subjects (86 male, 110 female) were enrolled, with a mean age of 76 years. In all subjects the diagnosis of BP was established by histological analysis of skin biopsies demonstrating subepidermal blistering and linear deposition of immune reactants (IgG and/or C3) along the BMZ junction. Usually, there were no previous treatments as only patients with acute onset of BP were treated. TMPT activity was never measured prior to initiation of AZA (Table 5)
Efficacy
Beissert et al. compared methylprednisolone plus AZA with methylprednisolone plus mycofenolate mofetil. Results show that in both groups a 100% remission was achieved. Time to remission was more prompt in the AZA group, although this was not statistically different. Cumulative dose of oral steroids and duration until relapse after tapering the medications were not significantly different between the two groups. In the study of Guillaume et al. prednisolone monotherapy was compared with prednisolone plus AZA and prednisolone plus plasma exchange. The study was interrupted after the interim analysis showed that there was neither an appreciable benefit resulting from addition of AZA or plasma exchange to prednisolone nor that this could be expected on completion of the study.
Burton et al. found a significant reduction (45%) of the cumulative prednisone dose over a 3 years period when comparing prednisolone monotherapy with prednisolone plus AZA. Although the percentage of remissions and numbers of deaths favored the oral corticosteroids plus AZA group, there was no significant difference between the groups.
After withdrawal of concomitant oral corticosteroids, duration of remission of the lesions was approximately 5.5 months on AZA monotherapy. Onset of action was never mentioned (Table 6.).
Cohort
Methodological quality
One cohort study by Ahmed et al. was included. Concerning the methodological quality a few remarks can be made. Firstly, demographic information about the individual treatment groups is missing. Therefore, a selection bias could not be excluded. Secondly, the two treatment groups were not comparable in terms of disease severity. Thirdly, some outcome data (length of hospitalization) mentioned in the methods section were not addressed in the results section. Fourthly, the method of outcome assessment was not validated and not blinded for the treatment arm.
Demography
Two groups were compared; prednisone and prednisone plus AZA. Twenty-nine subjects participated, 43-92 years of age. Subjects were not previously treated with other medication. The dosage of AZA employed was 1.5 mg/kg/day. Prednisone was given in reduction schedule after clinical remission occurred. The individual or mean duration of treatment was not reported. Follow up ranged from 8 to 45 months (Table 5).
Efficacy
A 50% reduction in maintenance dose of prednisolone dose was found in the AZA group and a 30% reduction in the length of systemic therapy. Whether these outcomes were statistically significant, is uncertain (Table 6).
Case series
Demography
Three studies with case series were included concerning 17 BP patients. Diagnosis of BP was histologically proven in all studies. The age of the subjects ranged from 47 to 91 years. Previous treatments were oral steroids. Van Dijk et al. was the only study in which AZA was used without concomitant prednisolone.
Burton et al. conducted a 4 years follow-up study monitoring the same subjects that were initiated on treatment during the Greaves et al. study. Two subjects were lost to follow up. The dose employed was 2.5 mg/kg/day in two studies and ranged from 75 to 250 mg/day in the third. Duration of treatment varied from 2 to 48 months and the follow-up period could be as long as 48 months (Table 5).
Effectiveness
Greaves et al. found that the dose of prednisolone at which the subjects relapsed (e.g. the relapse dose) was lower when subjects were using concomitant AZA. They found that by giving AZA it was possible to withdraw prednisolone maintenance treatment without relapses in 9 out of 11 subjects.
In the follow-up study by Burton et al. 4 of the above mentioned subjects remained in remission during 4 years, 1 became refractory, 1 experienced a moderate response and 4 subjects died.
Van Dijk et al. showed a very good response (no new blisters) in 2 subjects, a good response (occasional new blisters) in 2 subjects and one patient withdrew after 2 weeks because of a deterioration of the renal function by pre-existent renal disease. Time to response was 4-6 weeks (Table 6).
- 1 - Ahmed AR, Maize JC, Provost TT et al. Bullous pemphigoid. Clinical and immunologic follow-up after successful therapy. Arch Dermatol 1977; 113: 1043-6.
- 2 - Beissert S.Werfel. A comparison of oral methylprednisolone plus azathioprine or mycophenolate mofetil for the treatment of bullous pemphigoid. Arch Dermatol 2007; 143: Dec.
- 3 - Burton JL, Greaves MW, Burton JL et al. Azathioprine for pemphigus and pemphigoid--a 4 year follow-up. Br J Dermatol 1974; 91: 103-9.
- 4 - Burton JL, Harman RM, Peachey RD et al. A controlled trial of azathioprine in the treatment of pemphigoid proceedings. Br J Dermatol 1978; 99: 14.
- 5 - Jordon RE, Beutner EH, Witebsky E, Blumental G, Hale WL, Lever WF. Basement zone antibodies in bullous pemphigoid. JAMA. 1967 May 29;200(9):751-6.
- 6 - Greaves MW, Burton JL, Marks J et al. Azathioprine in treatment of bullous pemphigoid. Br Med J 1971; 1: 144-5.
- 7 - Guillaume JC, Vaillant L, Bernard P et al. Controlled trial of azathioprine and plasma exchange in addition to prednisolone in the treatment of bullous pemphigoid. Arch Dermatol 1993; 129: 49-53.
- 8 - van Dijk TJ, van Velde JL, van Dijk TJ et al. Treatment of pemphigus and pemphigoid with azathioprine. Dermatologica 1973; 147: 179-85.
Beoordelingsdatum en geldigheid
Publicatiedatum : 30-08-2014
Beoordeeld op geldigheid : 22-06-2010
A guideline can only be leading, if it is maintained on a continuous base, with systematic monitoring of medical scientific literature as well as regular contributions from clinical practice. In case of important developments, it can be decided that the complete working group shall meet to propose amendments, which will be distributed among the various professional groups. A revision will be planned at least every five years.
Doel en doelgroep
Objective
A guideline is a document with recommendations to support patient care in daily practice. The guideline is based on results of scientific research and subsequent formation of opinion, aimed at deciding on the appropriate medical intervention. A guideline and the documents derived from it, give recommendations for the treatment of patients, including psychosocial care and patient information.
Intended users
The guideline is intended for members of the medical and paramedical professional group, including: dermatologists, general practitioners, pharmacists and dermatology nurses, nurse practitioners and physician assistants. A text derived from the guideline is available for patients.
Samenstelling werkgroep
A working group was appointed for the development of the guideline. This group consisted of dermatologists, pharmacists and a general practitioner from Lareb (the Dutch pharmacovigilance centre). During the formation of the group, the geographical distribution of its members was taken into account as well as a balanced representation of academic and non-academic employment . The members of the working group have acted independently and not a single member received any favour aimed at influencing the guidelines.
|
J.G. (Jan Gerrit) van der Schroeff, MD, PhD |
Dermatologist, Chairman working group |
|
J.J.E. (Jannes) van Everdingen, MD, PhD |
Director NVDV |
|
M. E. (Mandy) Schram, MD |
PhD candidate and resident Dermatology |
|
P. (Pieter) van der Valk, MD,PhD |
Dermatologist |
|
W.R. (William) Faber MD. PhD, FRCP |
Dermatologist |
|
A.Y. (Amber) Goedkoop, MD, PhD |
Dermatologist |
|
R.J. (Rinke) Borgonjen, MD |
PhD candidate |
|
A. (Annemieke) Horikx, PharmD |
Pharmacist KNMP |
|
E.P. (Eugène) van Puijenbroek, MD |
General practitioner Lareb |
|
R.I.F. (Rutger) van der Waal, MD, PhD |
Dermatologist |
|
A. (Annemieke) Floor, PharmD |
Pharmacist-researcher |
|
W. (Wouter) Goldtschmidt, MD, PhD |
Dermatologist |
|
E.L. (Noortje) Swart PhD |
Clinical pharmacist |
|
Ph. I. (Phyllis) Spuls, MD, PhD |
Dermatologist |
Belangenverklaringen
List of conflicts of interest
None reported
Methode ontwikkeling
Evidence based
Implementatie
During the various phases of developing the draft guideline, the implementation of the guideline and the actual workability of the recommendations are taken into account as much as is possible. The guideline is distributed to all relevant professional groups and hospitals through the internet and in various medical journals attention will be given to the guideline.
Werkwijze
During a period of year ( meetings) the working group worked on a draft guideline. An expert group made a bottleneck analysis during the preparatory phase. The expert group compiled a list of drugs which are frequently subscribed for off-label use in dermatology. The listed drugs were prioritized according to frequency of use and occurrence of potential serious adverse events. The members of the working group had the opportunity to propose alterations in the list of selected drugs The members of the working group agreed on composing a guideline about the off-label use of the following six selected drugs:
- Azathioprine
- Cyclosporine
- Methotrexate
- sulfasalazine dapsone
- Hydroxychloroquine
The working group agreed that the outcomes efficacy/effectiveness and safety are crucial for decision making. . The working group started by making a draft guideline for azathioprine and decided that the applied methods would serve as a blueprint for the other five drugs. Useful literature was found by systematic searches and by checking of references (see “Methodology of literature search”). The members of the working group assessed the relevant literature with regard to content and quality. Subsequently, conclusions were drawn and recommendations were made for off-label use of the selected drugs by the members of the working group. The final version of the guideline was approved by all scientific societies involved on.
Methodology of literature search
Research question
For each selected drug a research question according to PICO was made.
PICO stands for:
- Participants/population: population of patients with a dermatological disease who are treated with a drug that is not registered for the use in this particular disease.
- Intervention: the selected drug.
- Comparison: any other treatment (e.g. other systemic therapy, placebo, quality of life intervention), in case of lack of a control group; no other treatment.
- Outcome: safety and/or efficacy.
Search strategy
For each selected drug a standardized search was performed in the Medline (by PubMed) (1950-2009), EMBASE (1980-2009) and CENTRAL databases. This search strategy was designed by a literature specialist of the department ‘Professionele Kwaliteit van de Orde van Medisch Specialisten’. Also references of included articles were screened for eligibility.
Pre-selection with keywords
After the searches were uploaded in Reference Manager, articles labeled with possible keywords for exclusion were selected. A sample was taken of these selected articles to check if there were any relevant articles in that selection. The sample size was either 20 or 50 articles, depending on the number of articles labeled with a specific keyword. If the sample didn’t contain any relevant articles, all the articles labeled with a specific keyword were excluded.
In the searches of cyclosporine, methotrexate, dapsone, hydroxychloroquine and sulfasalazine articles with the keywords ‘case report’ were excluded after a sample of 50 articles didn’t reveal any relevant articles for inclusion.
In addition, articles with the following keywords were excluded after a sample of 20 articles didn’t show any relevant articles:
|
Cyclosporine |
Dapsone |
||
|
- |
Transplantation |
- |
Leprosy |
|
- |
Transplantation immunology |
- |
Mycobarterium leprae |
|
- |
Transplantation immunology [Physiology] |
- |
Pneumocystis carinii |
|
- |
Acute graft rejection [Complication] |
- |
Toxoplasmosis |
|
- |
Acute graft rejection [Diagnosis] |
- |
Spider |
|
- |
Acute graft rejection [Drug therapie] |
Methotrexate* |
|
|
- Acute graft versus host disease |
- |
Psoriasis |
|
|
- |
Bone Marrow Transplantation |
- |
Reumathoid arthritis |
|
- |
Breast cancer |
- |
Leukemia |
|
- |
Graft Survival |
- |
Osteosarcoom |
|
- |
Graft Recipient |
- |
Lymphoma |
|
- |
Kidney Graft |
- |
Bladder |
|
- |
Kidney Transplantation |
- |
Breast Cancer |
|
- |
Liver Transplantation |
- |
Mycosis |
|
- |
Proteinuria |
- |
Multiple sclerosis |
|
- |
Nephritis |
- |
Colitis |
|
- |
Irradiation |
- |
Asthma |
|
- |
Heart transplantation |
- Cancer + skin + cutaneous |
|
|
- |
Vitamin |
Sulfasalazine |
|
|
- |
Psoriasis |
- |
Rheumatoid arthritis |
|
Hydroxychloroquine: |
- |
Arthritis |
|
|
- |
Rheumatic disease |
- |
Crohn |
|
- |
Systemic lupus erythematodes |
- |
Ulcerative colitis |
|
- |
Discoid lupus erythematodes |
|
|
|
- |
Lupus erythematosus |
|
|
* In the methotrexate search articles with the note ‘review’ were excluded after a sample of 20 articles didn’tcontain any relevant articles.
An overall validation of this method was provided by the double search strategy on azathioprine. An initial/broad search (thus without using keywords) was compared with the search that used specific keywords for exclusion. Articles with the keywords ‘case report’, ‘polymyositis’ and ‘idiopatic thrombocytopenic purpera’ were excluded after a sample showed no relevant articles.
We found that all studies that were included in initial/broad search were present in the search using keywords for exclusion. This validates the method of excluding articles by using keywords.
Selection of articles
All articles with title and abstract referring to off-label treatment with the predefined drug in patients with dermatological diseases were selected. To determine eligibility, the full text of the selected articles was screened according to the predefined in-and exclusion criteria. Data on methodological quality, study characteristics, efficacy and safety were extracted by using a data extraction form. All stages of literature selection and data extraction were performed by two independent reviewers. Disagreements about study selection and data extraction were solved by discussion.
In- and exclusion criteria
Selection of the articles was performed by using the following pre-defined in- and exclusion criteria. Inclusion criteria:
- The article concerns the selected drug and
- The selected drug is used in the treatment of a dermatological disease for which that particular drug is not registered.
Exclusion criteria:
- Case reports with less than 5 subjects*
- Lack of data on safety and efficacy
- Articles concerning treatment other than systemic treatment with the selected drug
- Animal studies
- In vitro studies
- Double publications
- Articles concerning diseases that are primarily treated by other specialists
- Language other than English, French, German and Dutch
No restrictions were imposed regarding age, gender, skin type and number of subjects in a study and date of publication.
* A random sample of the excluded articles was taken to check if any relevant adverse effects were missed.
Data-extraction
Of all the included articles, data were extracted by two independent reviewers. This was done by using a standardized data extraction form. Disagreements on data extraction were solved by discussion.
Data- extraction was performed on:
- Methodological quality
- Demographics
- Efficacy
- Safety
Methodological quality
Randomized controlled trials (RCT’s) were assessed following the criterion grading system described in the Cochrane Handbook for systematic reviews of interventions 5.0.0 (updated February 2008). To assess the risk of bias withinincluded RCT’s, the following parameters for methodological quality were used; sequence generation, concealment of allocation, blinding (of participants, researchers and outcome assessment), reporting of incomplete data, presence of selective outcome reporting and other potential threats to validity.
The methodological quality of cohort studies was assessed by using the checklists for cohort studies described by the Dutch Cochrane Centre.
Demographics
Data of demographics were extracted concerning:
- Study design: randomized? controlled? prospective, retrospective?
- Treatment arms
- Disease of the subjects: severity, stage, subtype, duration
- Previous medications
- Diagnostics: what was the method of diagnosis? Clinical, histopathological, other diagnostic criteria?
- Subjects: number, male/female, age, subgroups
- Duration of treatment
- Duration of follow up
- Concomitant medication
- Dosing schedule of the selected drug
Efficacy/effectiveness
- Used outcome parameters: clinical assessment, global assessment, quality of life measurement, laboratory markers, onset of effect, duration of remission, relapse rate, etc)
- Severity outcomes: the result of the used outcome parameters. Differences between baseline and end of the study and between treatment groups.
Safety
Safety is an important issue in off-label use of medication. The working group scored all adverse events, including a special focus on serious adverse effects. Within the included studies, every study that reported (serious) adverse events was taken into account. Adverse events reported in RCT’s or cohorts will be compared with the adverse events that occurred in the control group. If possible a relative risk will be calculated.
Extracted safety data:
- Adverse events: which? how many? at what time during treatment or after treatment?
- Serious adverse events: which? how many? at what time during treatment or after treatment?
- Withdrawals due to adverse events?
An Adverse Event (AE) was defined as an unfavorable and unintended sign, including an abnormal laboratory finding, symptom or disease associated with the use of a medical treatment or procedure, regardless whether it is considered related to the medical treatment or procedure, that occurs during the course of the study.
A Serious Adverse Events (SAE) was defined as any untoward medical occurrence that results in death, is life threatening, requires inpatient hospitalization or prolongation of existing hospitalization, results in persistent or significant disability/incapacity, is a congenital anomaly/birth defect or is reported in the study as such.
Handling of the data
Extracted data will be presented in tables and with accompanying text per disease following standardized means.
Level of evidence
The description and assessment of the articles according to the data extraction (see above) are listed in separate sections under the headers “Safety data off -label azathioprine” or “Efficacy/effectiveness data off-label azathioprine” and in tables (see section Tables).
Not all data extracted from articles are equally valuable. Therefore every set of articles is summarised in a conclusion, in which the level of the evidence is indicated according to the GRADE system (see boxes below). Consequently the recommendations in this guideline are based on evidence generated by scientific research, with emphasis on the outcomes safety and effectiveness/efficacy. The search results that were used are up to date until at least 01-10-2009, unless stated otherwise.
GRADE system
|
Type of evidence |
Randomized trial = high Observational study = low Any other evidence = very low |
|
Decrease* grade if |
Important inconsistency • Some or major uncertainty about directness • Imprecise or sparse data • High probability of reporting bias • Serious or very serious limitation to study quality |
|
Increase grade if |
• Strong evidence of association—significant relative risk of > 2 ( < 0.5) based on consistent evidence from two or more observational studies, with no plausible confounders (+1) • Very strong evidence of association—significant relative risk of > 5 ( < 0.2) based on direct evidence with no major threats to validity (+2) • Evidence of a dose response gradient (+1) • All plausible confounders would have reduced the effect (+1) |
|
*Each quality criterion can reduce the quality by one or, if very serious, by two levels. |
|
|
Conclusion
|
Development of the recommendations
For the development of a recommendation, other aspects than scientific evidence are also of importance, such as: patient preferences, availability of special techniques or expertise, organisational aspects, social consequences or costs. Known adverse events are also taken into account, as far as they were not already distilled from scientific literature. These aspects are discussed after the conclusion(s). On the basis of literature, the conclusion is here placed in the context of daily practice, and the pros and cons of the various treatments are balanced against each other. The final formulated recommendation is the result of the available evidence in combination with these considerations and can be formulated as a weak or strong recommendation in favour of a certain therapy or as a weak or strong recommendation against a certain therapy (see box below). The aim of this procedure and the formulation of the guideline using this ‘format’ is to enhance the transparency of the guideline. It leaves room for an efficient discussion during the meetings of the working group and moreover, it improves clarity for the user of the guideline.
|
Recommendation
|
Zoekverantwoording
Literature search
Between September 2009 and October 2009, a literature search in Medline (1950-2009), EMBASE (1980-2009) and CENTRAL was performed. As main search strategy ‘azathioprine’ and synonyms (not the active metabolites) were used in combination with all skin diseases; for example the search strategy in Medline:
1 derm*.jn. (22039)
2 Azathioprine/ (11859)
3 (azathioprine* or imuran* or immuran* or imurel*).ab. (8887)
4 (azathioprine* or imuran* or immuran* or imurel*).ti. (2856)
5 (azathioprine* or imuran* or imurel* or immuran*).kw. (72)
6 4 or 2 or 5 or 3 (16781)
7 6 and 1 (72)
8 exp Skin Diseases/ (669358)
9 6 and 8 (1705)
10 7 or 9 (1711)
11 limit 10 to (humans and (dutch or english or french or german)) (1535)
There was no limit with respect to the date of the publication. Literature references of all relevant articles found were checked in order to find additional articles. In addition, data published in Micromedex concerning azathioprine was studied to retrieve further potential relevant references regarding safety in off-label use. None were found.
Study selection and data extraction
All articles with title and abstract referring to off-label treatment with azathioprine of patients with dermatological diseases were selected by two reviewers. Next, to determine eligibility, the full text of the selected articles was screened by two reviewers. Disagreements were solved by discussion. Predefined in- and exclusion criteria are described in detail in the introduction section. Data on methodological quality, demographics, efficacy and safety were extracted by two independent reviewers using a data extraction form. Disagreements about data extraction were solved by discussion.
