Provisional treatment of soft tissue injury
Question
How should soft tissues be provisionally cared for in open fracture of the lower limb?
Subsidiary questions
- What are the benefits/disadvantages of short-term treatment of soft tissues with negative pressure therapy versus saline-soaked gauze in patients with a grade III open fracture of the lower limb?
- What are the benefits/disadvantages of short-term treatment (≤7 days) of the soft tissues with negative pressure therapy or saline-soaked gauze on comparison with longer-term treatment of the soft tissues in patients with a grade III open fracture of the lower limb?
Recommendation
Negative pressure therapy is the treatment of preference as a temporary wound cover as it helps to prevent infections and aids patient comfort.
If negative pressure therapy is not technically possible, the second choice is saline-soaked gauze dressings which have then been wrung out.
The application of a temporary wound cover should not deter the early and definitive covering of soft tissues.
The decision to continue temporary wound dressings for longer than one week is one that should be made in the primary multidisciplinary team.
Considerations
There are indications that there is an association between reduction in infection and the use of negative pressure therapy on comparison with saline-soaked gauze. There were also indications that negative pressure therapy should not be used for more than a week. The strength of evidence to support these finding has been graded very low. Until definitive coverage, one of the treatment goals is the prevention of infection. Infection occurs in the acute phase (0 to 72 hours) in 0 to 30% of cases. After 72 hours this percentage rises to 0 to 54% (Schlatterer, 2015). The only way to prevent the progression of infection is stable coverage. If definitive soft tissue treatment is postponed and not carried out directly, then wounds should be temporarily covered using saline-soaked gauze or negative pressure therapy. This enables treating physicians to plan definitive stabilisation and cover. Furthermore, in a polytrauma it gives the patient time for recovery from other traumas. Another aim of temporary coverage is to reduce the bacterial load and prevent new colonisation from the surface.
The advantage of negative pressure therapy over saline gauze is it creates a physical barrier in the form of an adhesive layer of plastic, which the saline gauze dressing lacks. Negative pressure systems also deliver active wound drainage whereas a saline gauze dressing has to be changed at intervals in order remove the bacteria-containing exudate. Finally, it is user-friendly for the nursing staff and the patient and reduces the number of daily wound care procedures required thus also costs. It is also much better for the patient as changing dressings is often painful.
Negative pressure therapy will only work if the vacuum is adequate. In cases where an external fixator is being used for temporary stabilisation, it is generally rather difficult to maintain a vacuum due to leakage of air from around the pins of the fixator. If this vacuum cannot be maintained, then due to the plastic barrier the negative pressure system changes to become a potential source of information resulting from stasis of the exudate and bacteria. Should the system continue to dysfunction it should be removed as soon as possible to avoid becoming a potential source of infection. In these cases, this may be a reason to primarily choose saline gauze dressings.
A temporary wound cover may only be applied with a specific aim in mind and should not be regarded as a reason not to carry out early coverage. If definitive coverage has not taken place within one week, the risk of infection probably increases. For this reason, a multidisciplinary team should discuss the desirability of prolonging temporary coverage.
Evidence
Background
There are several modalities for wound cover between initial debridement and definitive cover; these vary from saline-soaked gauze to antibiotic-impregnated beads covered with a membrane, and negative pressure therapy.
In principle, a provisional wound cover should only be regarded as temporary and should not delay permanent coverage. A delay of longer than one week between trauma and definitive fixation and coverage leads to a doubling of infection percentages of the fixation material and also to more complications associated with the soft-tissue reconstructive procedure.
Negative pressure therapy has become very popular over recent years. There are a number of arguments in favour of its use. It is user-friendly for the patient and nursing staff, and as well as providing temporary soft-tissue cover, it also facilitates the drainage of wound exudate. The extent to which these systems are better able to reduce bacterial load, thereby lowering the risk of infection, than more traditional methods of dressing is important when choosing between them.
Conclusions / Summary of Findings
Time to wound healing
|
Very low GRADE |
There are indications that negative pressure therapy may shorten time to recovery.
Source (Rasool, 2013) |
Infection reduction in the acute phase (<72 hours)
|
Very low GRADE |
There are indications that there is an association between reduction in infection and the use of negative pressure therapy on comparison with saline-soaked gauze.
Source (Schlatterer, 2015) |
Number of flap procedures following long-term (>72 hours) use of negative pressure therapy.
|
Very low GRADE |
There are indications that the use of negative pressure therapy leads to a reduction in the number of flap procedures required compared with treatment with wet gauze.
Source (Schlatterer, 2015) |
Risk of infection associated with long-term (>72 hours) use of negative pressure therapy.
|
Very low GRADE |
There are indications that prolongation of negative pressure therapy by three to seven days is associated with risk of infection equal to that of saline-soaked gauze. Using negative pressure therapy for longer than seven days may possibly increase the risk of infection.
Source (Schlatterer, 2015) |
Literature summary
Description of studies
Schlatterer’s review (2015) examined three aspects of negative pressure therapy in patients with a grade IIIB open tibial fracture. First, the risk of infection and the number of free-flap procedures associated with negative pressure therapy was compared with the use of wet saline-gauze dressings. They also compared the difference in the number of infections associated with short-term and long-term temporary wound cover. The review contains thirteen studies: one RCT and twelve retrospective studies. After the update, the randomised trial of Rasool (2013) was added. This study comprises 50 patients (35 men; 70%), with Gustilo type II, IIIA and IIIB open tibial fractures, who were randomised to a negative pressure therapy treatment group (n=25) or to a group treated with normal saline dressings (n-25). Time to wound healing (100% granulation) in both groups was then compared. The review defined infection as each patient who was treated with antibiotics or who underwent surgical incision and drainage.
Wound healing
Rasool 2013 examined the difference in time to wound healing between negative pressure therapy and saline-soaked gauze in 50 patients. Time to wound healing is defined at the number of days until 100% wound granulation was achieved. The results showed that negative pressure therapy gave a significantly greater chance of healing within 10-20 days than saline-soaked gauze dressings (RR=21.00; 95% CI 3.05 to 144.39; p<0.05).
Strength of evidence of the literature
The strength of evidence for the outcome ‘time to wound healing’ was lowered by three levels, taking into account the limitation of the study set-up and the extremely limited number of patients.
1. What are the benefits/disadvantages of short-term treatment of the soft tissues with negative pressure therapy on comparison with saline-soaked gauze in patients with a grade III open fracture of the lower limb?
Infection reduction in the acute phase (<72 hours)
Four studies from the review (one RCT and three observational studies) compared reduction of infection in patients treated by negative pressure therapy with patients treated by saline-soaked gauze (total n=461; negative pressure therapy n=332, infections n=47; saline-soaked gauze n=129, infections n=27). The RCT of Stannard found a statistically significant difference favouring negative pressure therapy (RR= 0.41; 95% CI 0.20 to 0.82). The two observational studies also found an association favouring negative pressure therapy (Blum 2012 RR=0.20; 95% CI 0.05 to 0.90; Parrett 2006 RR=0.48; 95% CI 0.18 to 1.27). Conversely, Liu (2012) found an increased risk (RR=3.69; 95% CI 0.93 to 14.55). The pooled effect (random effects model) gives an RR of 0.60 (95% CI 0.22 to 1.63) in favour of negative pressure therapy (heterogeneity (I2)= 71%). Infection risk varied from 5.4% to 29% in patients treated with negative pressure therapy and from 8.0 to 28.0% in patients treated with saline-soaked gauze.
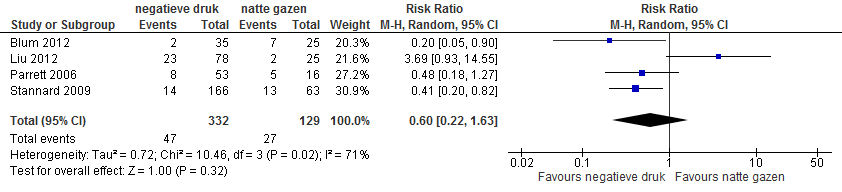
Figure 1 Forest plot of the pooled data: temporary coverage by means of negative pressure therapy gives a slight reduction of the number of wound infections on comparison with saline-soaked gauze.
Strength of evidence of the literature
The strength of evidence for the outcome ‘risk of infection’ was lowered by three levels, taking into account the contradictory results/large heterogeneity (inconsistency) and the limited number of patients.
No outcomes on osteitis, osteomyelitis, pain or patient satisfaction were reported.
2. What are the benefits/disadvantages of short-term treatment (≤7 days) of the soft tissues with negative pressure therapy or saline-soaked gauze on comparison with long-term treatment of the soft tissues in patients with a grade III open fracture of the lower limb?
Results
Six studies described the number of flap procedures that were necessary after negative pressure therapy compared with saline-soaked gauze (Bhattacharyya, 2008; Dedmond, 2006; Dedmond, 2007; Hou, 2011; Liu, 2012; Parrett, 2006). Parrot’s study (2006) showed a drop in the number of free-flap procedures following the introduction of negative pressure therapy from 42% to 11%. However, the number of local flap procedures remained the same and the necessary wound care (skin grafts and/or delayed primary or secondary wound closure) rose from 22% to 49%. The other five studies found a drop of 13% to 60% in the number of flap procedures on comparison with the years prior to the introduction of negative pressure therapy.
Strength of evidence of the literature
The strength of evidence for the outcome was lowered by three levels, taking into account the limitation of the design of the review and the limited number of patients (imprecision). Additionally, the number of flap procedures is a very indirect measure of the outcomes infection, osteitis and osteomyelitis.
The risk of infections in long-term negative pressure therapy
Results
Ten studies described the risk of infections in long-term negative pressure therapy. In these, the risk of infection varied between 0 and 54%. The review wanted to compare temporary wound cover of less and more than 72 hours, but the studies included used other cut-off points. The duration of negative pressure therapy varied between seven to 53 days. Bone stabilisation methods (external/internal) also varied between studies. This means it is difficult to ascertain if the outcomes are a result of the treatment or of the indication (selection bias). In eight of the ten studies, a raised risk of infection was found in patients who underwent long-term treatment with negative pressure therapy. In two of the ten studies (Hou, 2011 and Battacharyya, 2008), a raised risk of infection was found in the application of long-term negative pressure therapy compared with saline-soaked gauze. No quantitative data were available.
Strength of evidence of the literature
The strength of evidence was not graded with GRADE as no quantitative data were available to make a comparison between short-term and long-term application of temporary wound coverage.
Search and select
In order to answer this clinical question a systematic literature analysis was carried out in order to answer the following scientific questions:
What are the benefits/disadvantages of short-term treatment of the soft tissues with negative pressure therapy on comparison with saline-soaked gauze in patients with a grade III open fracture of the lower limb?
P: Patients with a grade III open fracture of the lower limb
I: Wound treatment with negative pressure therapy
C: Wound treatment with sterile gauze soaked in a saline solution.
O: Wound healing, infection, osteitis, osteomyelitis, pain, patient satisfaction
What are the benefits/disadvantages of short-term treatment (≤7 days) of the soft tissues with negative pressure therapy or saline-soaked gauze in patients with a grade III open fracture of the lower limb?
P: Patients with a grade III open fracture of the lower limb
I: Short-term (≤7 days) temporary wound cover such as negative pressure therapy or wet dressings
C: Long-term (>8 days) temporary wound cover such as negative pressure therapy or wet dressings
O: Wound healing, infection, osteitis, osteomyelitis, pain, patient satisfaction
Method of searching and selection
The databases Medline (OVID) and Embase were searched for systematic reviews using relevant search terms and randomised controlled studies and controlled studies (RCT and CCT). The search strategy is shown under the tab Justification.The literature search resulted in 191 hits. We first looked for a suitable systematic review that satisfied the PICO for this evidence synthesis. Reviews were included if they had searched at least two databases and the results were described transparently. The review that satisfied the criteria was updated with studies obtained from the search related to this clinical question. Studies were selected on the grounds of the following selection criteria: controlled research carried out in adults with a grade II/ III open fracture of the lower limb. Two additional studies were preselected on the basis of title and abstract. After reading the complete text, one study was excluded (see exclusion table) and one trial was definitively selected.
(Results)
One systematic review, containing one RCT and twelve retrospective studies, was included in the literature analysis. An update of the literature resulted in the addition of one RCT. The evidence tables and assessment of individual study quality can be found under the tab Evidence Base.
References
- Rasool G, Ahmed MU, Iqbal M. Vacuum assisted wound closure and normal saline dressing in treatment of Gustilo type II, type IIIa and IIIb open fracture of tibia. Rawal Medical Journal. 2013;38(4):382-384.
- Schlatterer DR, Hirschfeld AG, Webb LX. Negative pressure wound therapy in grade IIIB tibial fractures: fewer infections and fewer flap procedures? Clin Orthop Relat Res. 2015;473(5):1802-1811.
Evidence tables
|
Study reference |
Study characteristics |
Patient characteristics |
Intervention (I) |
Comparison (C) |
Follow-up |
Outcome measures and effect size |
Comments |
|
Schlatterer, 2015
|
SR of RCTs and retrospective studies
Literature search: SR: up to September 1, 2013 Update: up to April 15, 2015
A: Bhattacharyya, 2008 B: Blum, 2012 C: Dedmond, 2006 D: Dedmond, 2007 E: Hou, 2011 F: Karanas, 2008 G: Li, 2013 H: Liu, 2012 I: Liu, 2012 J: Parrett, 2006 K: Rinker, 2008 L: Stannard, 2009 M: Steiert, 2009 N: Rasool, 2013*
Study design: SR of a RCTs and retrospective studies
Country: SR: USA; Rasool 2013: Pakistan; Other studies: Unknown
Source of funding: Not stated
|
Inclusion criteria SR: negative pressure wound therapy, tibial fractures, open fractures, infections or osteomyelitis, muscle flap or flap procedures, English, humans, all levels of evidence, published between 2006 and September 2013 (SR) and up to April 15 2015 (update).
Exclusion: Review articles, pilon fractures, insufficient data or case reports
13 studies included
Important patient characteristics at baseline: A to M: No information on patient characteristics is not reported.
N: Age: 10-40 yrs. Gender: total: 35/50 male, 15/50 female: VAC group 68% male, saline dressings group 72% Wound size: mode 6 to 7.5 cm in VAC as well as saline dressings group Location of wound (high/middle/low shaft): total group n= 7/18/25; VAC n=3/10/12, saline dressings n=4/8/13
Groups comparable at baseline? A to M: Unknown N: yes |
A to N: VAC
|
A to M: gauze dressings N: Saline dressings
|
End-point of follow-up: Unknown N: number of days until appearance of 100% granulation tissue over wound.
For how many participants were no complete outcome data available? (intervention/control) Unknown
|
Time of wound healing (100% granulation tissue) Effect measure: RR [95% CI] N: 10-20 days: VAC 84%, saline dressings 4%; RR= 21.00 [3.05 to 144.39] 21-30 days: VAC 16%, saline dressings 48% 31-40 days: VAC 0%, saline dressings 48%; RR= 0.04 [0.00 to 0.64]
Infection risk in acute phase (<72hrs.) Effect measure: RR [95% CI] B: RR=0.20 [0.05, 0.90] I: RR=3.69 [0.93, 14.55] J: RR= 0.48 [0.18, 1.27] L: RR= 0.41 [0.20, 0.82] Pooled effect (random effects model; n=461): RR=0.60 [95% CI 0.22 to 1.63] favoring VAC Heterogeneity (I2): 71%
Infection rates after (>72 hrs.) Effect measure: RR [95% CI:
A: VAC 8/14, gauze dressings 3/24, RR= 4.57 [1.45, 14.46] C: NS D: NS E: VAC 10/22, gauze dressings 1/10, RR=4.55 [0.67, 30.85] F: NS G: NS H: NS I: NS K: NS M: NS
Infection rates after 7 days Effect measure: RR [95% CI] A: VAC 8/14, gauze dressings 3/24, RR= 4.57 [1.45, 14.46] E: VAC 10/22, gauze dressings 1/10, RR=4.55 [0.67, 30.85] Pooled effect (random effects model; n=70): RR=4.56 [95% CI 1.70 to 12.25] favouring gauze dressings Heterogeneity (I2): 0%
Flap procedure rates after >72 hrs. of negative pressure wound therapy Effect measure: RR, RD, mean difference [95% CI]: A, C, D, E, I: 13 to 60% decrease in flap rates J: free flap rate: VAC 11%, gauze dressings 42%; local flap rate: VAC 38%, gauze dressings 40 (NS); local wound care: VAC 22%, gauze dressings 49% |
Abbreviations: NS=Not significant VAC= negative pressure wound therapy or Vacuum-Assisted Closure therapy system SR= Systematic review RCT= randomized controlled trial RR=Risk ratio CI=Confidence interval
* The study Rasool 2013 was added to the review after update.
|
Risk of bias table for intervention studies (randomized controlled trials)
Research question:
|
Study reference |
Describe method of randomisation1 |
Bias due to inadequate concealment of allocation?2 |
Bias due to inadequate blinding of participants to treatment allocation?3 |
Bias due to inadequate blinding of care providers to treatment allocation?3 |
Bias due to inadequate blinding of outcome assessors to treatment allocation?3 |
Bias due to selective outcome reporting on basis of the results?4 |
Bias due to loss to follow-up?5 |
Bias due to violation of intention to treat analysis?6 |
|
Rasool, 2013 |
Alternation (quasi-random method of allocation) |
likely |
likely |
likely |
likely |
unclear |
unlikely |
unlikely |
Table Excluded after reading complete article
|
Author and year |
Reason for exclusion |
|
Cheng, 2013 |
No relevant comparisons were studied. |
Other evidence tables depending on type of clinical question.
Methods
Authorization date and validity
Last review : 01-01-2017
The executive board of the NVvH will assess these guidelines no later than 2020 to determine if they are still valid. If necessary, a new working party will be set up to review the guidelines. If there are new developments, the validity of the guidelines will expire earlier and a review will take place. The working party does not deem it necessary to separately specify validity at a modular level.
As owners of these guidelines, the primary responsibility to keep them up-to-date rests with the NVvH. Other participating professional bodies or users of the guidelines share the responsibility and are required to inform the NVvH about relevant developments in their fields.
General details
The development of these guidelines was financed by the Quality Foundation of the Dutch Medical Specialists (SKMS).
Scope and target group
What is the aim (desired effect) of the guidelines?
The recognition and acknowledgement of the complexity of a fracture of the lower limb with significant soft tissue injury is of the greatest of importance in developing an appropriate multidisciplinary treatment strategy. The specialisations involved must be very aware of their own abilities and limitations, and on the basis of these must work in partnership right from when the patient is first presented. Standardisation of therapeutic options by means of a treatment algorithm is necessary. The development of multidisciplinary, evidence-based guidelines contributes to this.
Currently, the treatment of an open lower limb fracture is not managed by a scientifically supported and multidisciplinary policy, but more likely by the local traditions of the hospital at which the patient presents. This often causes confusion about the most appropriate method of primary fixation, the timing and the extent of aggressiveness of the debridement and the planning for definitive coverage of the soft tissues.
In the Netherlands, there is currently no standardised treatment for patients with an open fracture of the lower limb. There are British guidelines on this injury (BAPRAS/BOA, 2009), but these are not always applicable to the Dutch situation for a number of reasons, including the differing ways in which care is organised. National, evidence-based guidelines are of considerable importance in supporting health care professionals in their clinical decision-making and in providing transparency to patients and third parties. It covers topics in several areas including the early and late treatment of open fractures of the lower limb, the timing and kind of surgical debridement, bone stabilisation, soft tissue cover and rehabilitation. The ultimate goal is to create a primary multidisciplinary treatment pathway whereby patients with complex open fractures of the lower limb can be treated quickly and to a high standard.
Defining the guidelines
The guidelines are aimed at all patients with an open fracture of the lower limb, and in particular at those patients with a grade III (a, b or c) open injury in accordance with the classification of Gustilo and Anderson. The principles of treatment described in these guidelines are also applicable to open fractures in other parts of the skeleton, such as the ankle.
Envisaged users of the guidelines
These guidelines have been written for all members of those professional groups who are involved in the medical care of adults or children with an open fracture of the lower limb: emergency department physicians, trauma surgeons, orthopaedic surgeons, plastic surgeons, rehabilitation physicians, physiotherapists, nurses and wound consultants.
Samenstelling werkgroep
In 2014, a multidisciplinary working party was set up to develop these guidelines. It comprised representatives from all those relevant specialisations involved in the care of patients with a grade III open fracture of the lower limb (see below).
The members of the working party were mandated for participation by their professional organisation. The working party worked for two years to develop these guidelines.
The working party is responsible for the integral text of these guidelines.
- Dr M.J. Elzinga, trauma surgeon (NVvH), Haga Hospital, The Hague (Chair)
- Dr J.M. Hoogendoorn, trauma surgeon (NVvH), Medical Centre Haaglanden-Bronovo, The Hague, The Netherlands.
- Dr P. van der Zwaal, orthopaedic surgeon (NOV), Medical Centre Haaglanden-Bronovo, The Hague, The Netherlands.
- Dr D.J. Hofstee, orthopaedic surgeon (NOV), Noordwest Hospital Group, The Netherlands
- J.G. Klijnsma, physiotherapist (KNGF), University Medical Centre Utrecht, The Netherlands
- Dr P. Plantinga, emergency department physician (NVSHA), Rijnstate Hospital, Arnhem, The Netherlands.
- Dr H.R. Holtslag, rehabilitation physician (VRA), Academic Medical Centre, Amsterdam, The Netherlands.
- Dr E.T. Walbeehm, plastic surgeon (NVPC), Radboud Hospital, Nijmegen, The Netherlands.
- Dr H.A. Rakhorst, plastic surgeon (NVPC), Medisch Spectrum, Twente, The Netherlands.
With the help of:
- Dr W.A. van Enst, senior advisor, Knowledge Institute of Medical Specialists
With thanks to:
- Dr C.W. Ang, medical microbiologist, VU Medical Centre, Amsterdam. The Netherlands.
Declaration of interest
The members of the working party have declared in writing if, in the last five years, they have held a financially supported position with commercial businesses, organisations or institutions that may have a connection with the subject of the guidelines. Enquiries have also been made into personal financial interests, interests pertaining to personal relationships, interests pertaining to reputation management, interests pertaining to externally financed research, and interests pertaining to valorisation of knowledge. These Declarations of Interest can be requested from the secretariat of the Knowledge Institute of Medical Specialists. See below for an overview.
|
Name of member of working party |
Interests: Yes/No |
Remarks |
|
M.J. Elzinga |
No |
|
|
Dr J.M. Hoogendoorn |
No |
|
|
Dr P. van der Zwaal |
Yes |
Member of an Orthopaedic & Traumatology partnership financially supported by Biomet in the interests of scientific research |
|
Dr D.J. Hofstee |
No |
|
|
Mr J.G. Klijnsma |
No |
|
|
P. Plantinga |
No |
|
|
Dr H.R. Holtslag |
No |
|
|
Dr E.T. Walbeehm |
No |
|
|
Dr H.A. Rakhorst |
No |
|
Patient involvement
The perspective of the patient was included by organising a focus group. This report can be found in the appendices. The concept guidelines was presented to the Patient Federation NPCF for their comments.
Method of development
Implementation
Introduction
This plan has been drawn up with the aim of advancing the implementation of these guidelines. In order to compile this plan, an inventory of factors that could either facilitate or hinder the recommendations was carried out. The guideline working group has made recommendations concerning the timeline for implementation, the preconditions necessary for this and the actions that should be taken by various parties.
Methodology
In order to arrive at this plan, the working party has applied the following to each recommendation in the guidelines:
- the time point by which the recommendations should have been nationally implemented;
- the expected impact of implementation of the recommendation on healthcare costs; preconditions necessary to be able to implement the recommendation; possible barriers to the implementation of the recommendation; possible actions to advance the implementation of the recommendation; the party responsible for the actions to be undertaken.
Readers of this implementation plan should take the differences between ‘strong’ recommedations and ‘weak’ recommendations into account. In the former case, the guideline committee clearly states what should or should not be done. In the latter case, the recommendation is less strong and the working party expresses a preference but leaves more room for alternatives. One reason for this could be that there is insufficient research evidence to support the recommendation. A weak recommendation can be recognised by its formulation and may begin with something like ‘Consider the…’. The working party has considered the implementation of both weak and strong recommendations. A time frame for implementation is only indicated for strong recommendations.
Time frames for implementation
Strong recommendations should be followed as strictly as possible. In most cases, this will mean that the recommedations should be implemented within one year of the publication of the guidelines.
However, some recommedations will not be directly implemented everywhere. This could be due to a lack of facilities, expertise or correct organisational structure. In some cases, account should be taken of the learning curve. In addition, the unavailability of staff or facilities or lack of agreement between professionals may hinder the implementation in the short term.
It is for these reasons that the following recommendations are based on estimates made by the guideline working group, and an implementation period of between one and three years should be allowed for:
|
Recommendation |
Remarks |
|
At the scene, treat patients with an open fracture of the lower limb in accordance with the Netherlands National Protocol of Ambulance Care (LPA) and Prehospital Trauma Life Support (PHTLS) principles.
|
Taking note of the guidelines is sufficient for implementation |
|
Take photographs of the injuries so the temporary dressing does not continually need to be disturbed (important for the privacy of the patient). |
Taking note of the guidelines is sufficient for implementation |
|
Assess the wound, vascular status and nerve injury and classify the injury in accordance with the Gustilo and Andersen classification. |
Taking note of the guidelines is sufficient for implementation |
|
Assess and describe the degree of contamination and the extent of the soft tissue injuries. |
Taking note of the guidelines is sufficient for implementation |
|
Repeat neurovascular status assessment paying special attention to the development of compartment syndrome and acute vascular threat to the leg. |
Taking note of the guidelines is sufficient for implementation |
|
Avoid taking wound cultures in the ED. |
Taking note of the guidelines is sufficient for implementation |
|
Take plain radiographs in two directions (AP and lateral) including the proximal and distal joints. |
Taking note of the guidelines is sufficient for implementation |
|
If peripheral pulsations are intact, then only carry out CT angiography on indication (clinical suspicion or preoperative work-up). |
Taking note of the guidelines is sufficient for implementation |
|
If the leg is acutely threatened surgical exploration and shunting be should carried out in order to keep acute ischaemic time to a minimum. The site of the vascular damage can be accurately determined using conventional radiological diagnostics and the level of the area of trauma. |
Taking note of the guidelines is sufficient for implementation |
|
In ED remove those contaminants that are easy to remove, and leave perforating objects (e.g. cables or slivers of metal or glass) in situ. |
Taking note of the guidelines is sufficient for implementation |
|
Wound irrigation should emphatically not take place in the ED. |
Taking note of the guidelines is sufficient for implementation |
|
Cover wounds with sterile gauze soaked in a saline solution. |
Taking note of the guidelines is sufficient for implementation |
|
Align dislocated fractures and apply a splint. |
Taking note of the guidelines is sufficient for implementation |
|
Intravenous antibiotics and a tetanus vaccination should be administered as early as possible in accordance with regional protocol. |
Taking note of the guidelines is sufficient for implementation |
|
Pain relief should be started as quickly as possible and in accordance with local protocol or guidelines on trauma patients in the emergency care pathway. |
Taking note of the guidelines is sufficient for implementation |
|
Debridement should be carried out systematically, working from skin to bone. If necessary, the wound should be lengthened along perforator-sparing fasciotomy lines in order to obtain a good overview of the affected area. Any further operations should be taken into consideration at this time and this should be discussed by the multidisciplinary team. |
Staff training, specifically aimed at the treatment of open fractures of the lower limb |
|
Irrigate under low pressure using plenty of saline solution. |
Staff training, specifically aimed at the treatment of open fractures of the lower limb |
|
Negative pressure therapy is the treatment of preference as a temporary wound cover as it helps to prevent infections and aids patient comfort. |
Staff training, specifically aimed at the treatment of open fractures of the lower limb |
|
If negative pressure therapy is not technically possible, the second choice is saline-soaked gauze dressings which have then been wrung out. |
Staff training, specifically aimed at the treatment of open fractures of the lower limb |
|
The application of a temporary wound cover should not deter the early and definitive covering of soft tissues. |
Dependent on the availability of enough adequately trained staff or on care arrangements with other hospitals. |
|
Aim to achieve primary internal fixation with nail or plate if good soft tissue cover is possible and the leg can be reasonably expected to bear weight.
|
Staff training, specifically aimed at the treatment of open fractures of the lower limb |
|
The working party neither recommends nor discourages primary bone grafting in open fractures. |
- |
|
As little research has been done in the area of primary bone grafting, for the time being this technique should be used in a study setting. |
Registration and permission from ethics committee to collect and study patient data should be organised. |
|
Definitive reconstruction of the soft tissues in open fracture of the lower limb should take place as quickly as possible, within a maximum of one week, if the condition of the patient permits this. |
Dependent on the availability of enough adequately trained staff or on care arrangements with other hospitals. Staff training, specifically aimed at the treatment of open fractures of the lower limb |
|
Keep as much length and tissue as possible and, where feasible, repair soft tissue injury with skin grafts. |
Taking note of the guidelines is sufficient for implementation Supplemented by further training |
|
Involve a rehabilitation physician as quickly as possible following the accident; preferably preoperatively to advise the patient. |
Taking note of the guidelines is sufficient for implementation |
|
If a transtibial amputation is not possible, carry out disarticulation of the knee in preference to transfemoral amputation. |
Taking note of the guidelines is sufficient for implementation |
|
When treating grade III open fractures, an antibiotic such as cefazolin which protects against Staphylococcus aureus should be given. |
Taking note of the guidelines is sufficient for implementation |
|
In grade III open fractures, antibiotics should be given until the soft tissues have been closed, preferably a maximum of 72 hours. |
Taking note of the guidelines is sufficient for implementation |
|
Consult a microbiologist on antibiotic therapy in the event of exceptional contaminants (marine, animal housing or sewerage). In grade III fractures consider adding an extra drug (e.g. an aminoglycoside such as tbramycin, gentamycin or ciprofloxacin), or using a third-generation cephalosporin (a potential disadvantage of these drugs being they are less effective against S aureus). |
Taking note of the guidelines is sufficient for implementation |
|
Consult a microbiologist on antibiotic therapy in the event of exceptional contaminants (marine, animal housing or sewerage). |
Taking note of the guidelines is sufficient for implementation |
|
Start exercise therapy as quickly as possible postoperatively. |
Taking note of the guidelines is sufficient for implementation |
|
Exercise therapy should be primarily aimed at disorders of function as specified in the ICF model (function of leg musculature, ROM of knee and ankle), and secondarily at activities (standing and walking). |
Taking note of the guidelines is sufficient for implementation |
|
In consultation with patient and surgeon set treatment targets for exercise therapy while taking the weight-bearing capacity of bone and soft tissues into consideration. |
Taking note of the guidelines is sufficient for implementation |
|
Over time, adapt these exercise therapy targets to the biological and mechanical possibilities and limitations of the wound, bone and soft tissues, the surgical procedure and potential complications. |
Taking note of the guidelines is sufficient for implementation |
|
Should quantification of physical functioning be called for, six-weekly WOMAC and SF-36 are recommended. |
Taking note of the guidelines is sufficient for implementation |
|
Return to work and quality of life are determined by personal and environmental factors. |
Taking note of the guidelines is sufficient for implementation |
|
If necessary, take measures to prevent talipes equinus. |
Taking note of the guidelines is sufficient for implementation |
|
Nominate a primary treating physician. |
Taking note of the guidelines is sufficient for implementation |
|
Make local or regional arrangements regarding the organisation of care for patients with a grade III open fracture of the lower limb and register this in a protocol. |
Taking note of the guidelines is sufficient for implementation |
|
Arrange to discuss the definitive treatment plan with the patient and family or close friends. Point out the possible treatment options, the risks associated with these options, and the expected results. |
Taking note of the guidelines is sufficient for implementation |
|
The meeting should be led by, or be held in the presence of, the primary treating physician. |
Taking note of the guidelines is sufficient for implementation |
The following recommendations are based on estimates made by the guideline committee, and an implementation period of between three to five years should be allowed for:
|
Recommendation |
Remarks |
|
The initial debridement should be done as quickly as possible, certainly within twelve hours of the initial trauma. It should be carried out by an experienced, trained and well-equipped multidisciplinary team. |
Hospitals should have enough staff available to be able to provide a multidisciplinary team, or they should have arrangements with other institutions who are able to provide care from a multidisciplinary team. |
|
The decision to continue temporary wound dressings for longer than one week is one that should be made by the primary multidisciplinary team. |
Hospitals should have enough staff available to be able to provide a multidisciplinary team, or they should have arrangements with other institutions who are able to provide care from a multidisciplinary team. |
|
Form a multidisciplinary team comprising a minimum of trauma surgeon/orthopaedic surgeon, a plastic surgeon and a rehabilitation physician. |
Hospitals should have enough staff available to be able to provide a multidisciplinary team, or they should have arrangements with other institutions who are able to provide care from a multidisciplinary team. |
|
The multidisciplinary team should see the patient preoperatively (rehabilitation physician if indicated) and together draw up a treatment plan. |
Hospitals should have enough staff available to be able to provide a multidisciplinary team, or they should have arrangements with other institutions who are able to provide care from a multidisciplinary team. |
Impact on healthcare costs
Many of these recommendations will have few or no consequences for the cost of healthcare. However, the deployment of a multidisciplinary team will possibly increase direct costs. Conversely, if the guidelines are adhered to the number of infections and reoperations will be reduced thus reducing costs. The savings are larger than the cost of the multidisciplinary team. Other recommendations do not affect costs, or may even save them.
Actions to be undertaken by each party
Below is a list of actions that in the opinion of the guideline working group should be undertaken to facilitate the implementation of the guidelines.
All academic and professional organisations that are directly involved (NVvH, NVPC, NOV, VRA, KNGF).
- Tell members about the guidelines. Publicise the guidelines by writing about them in journals and disseminating news of them at congresses.
- Provide professional education and training to ensure that the expertise required to follow the guidelines is available.
- Where relevant and possible, develop resources, instruments and/or digital tools to facilitate the implementation of the guidelines.
- Monitor the way in which the recommendations are put into practice by means of audits and quality inspections.
- Include indicators developed for these guidelines in quality registrations and indicator sets.
- Make interprofessional agreements about implementing continuous modular maintenance of the guidelines.
Initiatives to be undertaken by the professional organisation NVvH
- Hospital management boards and other system stakeholders (where applicable), should be kept informed of recommedations that could have an effect on the organisation of care and on costs, and on what may be expected by the party concerned.
- Publicise the guidelines to other interested academic and professional bodies.
Local professional groups / individual medical professionals
- Discuss the recommendations at meetings of professional groups and local working parties.
- Tailor local protocols to fit the recommendations from the guidelines.
- Follow the continuing professional education on these guidelines (yet to be developed).
- Modify local information for patients using the materials that the professional bodies will make available.
- Make agreements with other disciplines involved to ensure the implementation of the recommedations in practice.
- Register pre- and postoperative factors and, as far as is possible, include important considerations for decision-making in existing protocols and the electronic dossier.
The system stakeholders (including health insurers, NZA, hospital managers and their associations, IGZ)
In relation to the financing of care for patients with open fracture of the lower limb, it is expected that hospital management boards will be prepared to make the investments necessary to enable the implementation of these guidelines (see impact on healthcare costs above). In addition, hospital managers are expected to monitor those medical professionals concerned and ascertain how familiar they are with the new guidelines and how they are putting them into practice.
Health insurers are expected to reimburse the costs of the care that is prescribed in these guidelines. When the time frames for implementation have elapsed, health insurers can use the strong recommendations in these guidelines for purposes of purchasing care.
Researchers and subsidy providers
Initiate research into the knowledge gaps, preferably in a European setting.
Knowledge Institute of Medical Specialists
Publicise these guidelines among the staff and contect to development of related guidelines, e.g. on ankle fractures and post-osteosynthesis infection.
Add guidelines to guideline database. Incorporate this implementation plan in a place where all parties will be able to find it.
Methods and proces
AGREE II
These guidelines were developed in accordance with the publication Medical Specialists Guidelines 2.0 report from the advisory committee on Guidelines from the Committee on Quality. This report is based on the AGREE II instrument (Appraisal of Guidelines for Research & Evaluation II) (http://www.agreetrust.org/agree-ii/). This is a widely-accepted internationally used instrument and is based on ‘Guideline to guideline for the assessment of quality of guidelines (http://www.zorginstituutnederland.nl/).
Inventory of problem areas
During the preparation stage, the Chair of the Working Party and the Advisor made an inventory of problem areas. The Dutch health insurance companies were invited to contribute their problem areas to the guidelines.
Clinical questions and outcome measures
Based on the outcomes of the problem area analysis, the Chair and the Advisor compiled concept clinical questions. These were discussed with the working party, after which time the working party approved the definitive clinical questions. The working party then decided which outcome measures of each of the clinical questions are relevant to the patient, and both desirable and undesirable effects were examined. The working party then rated these outcome measures and categorised their relative importance as crucial, important or unimportant. In as far as was possible, the working party also defined what they found to be clinically relevant difference in the outcome measures, i.e. if the improvement in outcome was an improvement for the patient.
Strategy for searching and selecting the literature
For purposes of orientation, we looked for existing guidelines from outside the Netherlands (Guidelines International Network, Trip and National guideline clearing house (USA) European and American professional organisations), and systematic reviews (Medline, Embase, Cochrane Database of Systematic Reviews). Then, using specific search terms from the individual clinical questions, the working party searched for published studies in various electronic databases. Studies from the reference lists of the selected articles were also included in the search. Initially, studies with the highest level of evidence were searched for. The members of working party then went through the articles found in the search and selected articles based on predetermined selection criteria. The selected articles were used to answer the clinical questions. The databases searched, the search action or key words of the search action and the selection criteria used are defined in the search strategy of the clinical question concerned.
Quality evaluation of individual studies
In order to estimate the risk of bias in the study results, individual studies were systematically evaluated on the basis of previously determined methodological quality criteria. These evaluations can be found in the methodological checklists.
Summary of the literature
The relevant data from all studies included are shown in evidence tables. The most important findings from the literature were described in the summary of the literature. In the event of enough agreement between studies, the data were summarised quantitatively in a meta-analysis. This was done with Review Manager software from the Cochrane Collaboration.
Evaluation of the strength of scientific evidence
A) Intervention and diagnostic questions
Evaluation of the strength of scientific evidence was determined in accordance with the GRADE method. GRADE stands for ‘Grading Recommendations Assessment, Development and Evaluation’ (see http://www.gradeworkinggroup.org/) (Atkins, 2004).
GRADE distinguishes four grades of quality of evidence, i.e. high, moderate, low and very low. These grades indicate the degree of confidence in the conclusions in the literature (see http://www.guidelinedevelopment.org/handbook/).
|
GRADE |
Definition |
|
High |
|
|
Moderate |
|
|
Low |
|
|
Very low |
|
B) Questions concerning aetiology and prognosis
GRADE cannot be applied in this type of question. The strength of evidence of the conclusion is determined in accordance with the EBRO method (van Everdingen, 2004).
Formulating the conclusions
Evidence concerning questions about the value of diagnostic tests, injury or side effects, aetiology and prognosis, has been summarised in one or more conclusions in which the level of the most relevant evidence is given.
In questions relating to intervention and diagnosis, the conclusion does not refer to one or more articles, but is drawn on the basis of the whole body of evidence. In this the members of the working party did an analysis for each intervention. In making these calculations, the beneficial and unfavourable effects for the patient were weighed off against one other.
Considerations
In order to produce a recommendation, aspects other than research evidence are also important. These include the expertise of the members of the working party, patient preferences, costs, availability of facilities and organisational matters. In as far as they are not part of the literature summary, these aspects are reported under the heading ‘Considerations’.
Development of recommendations
The recommendations answer the clinical question and are based on the best available scientific evidence and the most important considerations. The strength of the scientific evidence and the weight accorded the considerations by the working party together determine the strength of the recommendation. In accordance with the GRADE methodology, a low grade of evidence from a conclusion in the systematic literature analysis does not exclude a strong recommendation, and a high grade of evidence does not exclude a weaker recommendation. The strength of the recommendation is always determined by weighing up all relevant arguments together.
Preconditions (Organisation of care)
In the analysis of problem areas and the development of the guidelines, account was taken explicitly of the organisation of care: all those aspects that are preconditions for the provision of care. These include coordination, communication, materials, financial means, work force and infrastructure. Preconditions that are relevant to the answering of a specific clinical question are part of the considerations related to that specific question.
Development of indicators
At the same time as the concept guidelines were developed, internal quality indicators were also developed in order to be able to follow and to strengthen the application of a guideline in practice. More information about the method of developing indicators can be requested from the secretariat of the Knowledge Institute of Medical Specialists (secretariaat@kennisinstituut.nl).
Knowledge gaps
In the development of these guidelines, we systematically searched for research whose results contributed to answering one of the clinical questions. The working party examined each clinical question and they considered the desirability of further research. An overview of their recommendations for further research can be seen in Knowledge gaps (see related products).
Comment and authorisation stage
To follow (after comment stage)
Implementation
At each stage of the development of the guidelines, account was taken of the implementation of the guidelines and the feasibility of the recommendations in practice. In this, particular attention was paid to factors that may advance or hinder the implementation of the guidelines.
Search strategy
|
Database(s): Medline, Embase |
Date: 15-04-2015 |
|
Period: 1995- present day |
Languages: E N |
|
Database |
Search terms |
Total |
|
Medline (OVID)
1995-April 2015
English, Dutch |
1 exp Lower Extremity/ (131744) 2 fibula/ or tibia/ (32404) 3 exp "Bones of Lower Extremity"/ (106996) 4 (tibi* or pilon or ankle* or fibula or talus or malleol* or foot or feet or forefoot or forefeet or 'below knee' or 'lower limb' or 'lower limbs' or 'lower leg' or 'lower legs' or toe* or shin* or 'lower extremity' or 'lower extremities' or crur*).ab,ti. (254028) 5 ankle fractures/ or tibial fractures/ (12729) 6 1 or 2 or 3 or 4 or 5 (404850) 7 Fractures, Open/ (4431) 8 ((open or mangled or "acute complex") adj4 (fracture* or trauma*)).ab,ti. or gustilo*.ab,ti,kw. or (exposed adj3 bone*).ti,ab. (8416) 9 7 or 8 (10633) 10 6 and 9 (4494) 32 Negative-Pressure Wound Therapy/ (1471) 33 exp Atmospheric Pressure/ (12631) 34 (((negative or Subatmospheric) adj3 pressure) or (vacuum-assisted adj3 closure*) or VAC).ti,ab. (10686) 35 32 or 33 or 34 (22826) 36 10 and 35 (76) 37 limit 36 to (yr="1995 -Current" and (dutch or english)) (64) 38 Bandages/ or (bandage* or dressing* or "topical therapy*" or "wound therap*").ti,ab. (30156) 39 32 or 33 or 34 or 38 (51414) 40 10 and 39 (146) 41 limit 40 to (yr="1995 -Current" and (dutch or english)) (96) – 95 uniek |
191 unique |
|
Embase (Elsevier) |
‘distal tibia fracture'/exp OR 'tibia shaft fracture'/exp OR 'proximal tibia fracture'/exp OR 'tibia fracture'/exp OR 'fibula fracture'/exp OR 'foot'/exp OR 'ankle fracture'/exp OR ((tibi* OR pilon OR ankle* OR fibula OR talus OR malleol* OR foot OR feet OR forefoot OR forefeet OR 'below knee' OR 'lower limb' OR 'lower limbs' OR 'lower leg' OR 'lower legs' OR toe* OR shin* OR 'lower extremity' OR 'lower extremities' OR crur*) NEAR/6 (fracture* OR defect*)):ab,ti OR 'tibia'/exp OR 'fibula'/exp OR 'talus'/exp OR 'tarsal bone'/exp OR 'toe phalanx'/exp OR tibi*:ab,ti OR pilon:ab,ti OR ankle*:ab,ti OR fibula:ab,ti OR talus:ab,ti OR malleol*:ab,ti OR foot:ab,ti OR feet:ab,ti OR forefoot:ab,ti OR forefeet:ab,ti OR 'below knee':ab,ti OR 'lower limb':ab,ti OR 'lower limbs':ab,ti OR 'lower leg':ab,ti OR 'lower legs':ab,ti OR toe*:ab,ti OR shin*:ab,ti OR 'lower extremity':ab,ti OR 'lower extremities':ab,ti OR crur*:ab,ti AND [english]/lim
AND ('open fracture'/exp OR ((open OR mangled OR 'acute complex') NEAR/2 (fracture* OR trauma*)):ab,ti OR gustilo*:de,ab,ti)
AND ('vacuum assisted closure'/exp OR 'hypobarism'/exp OR ((negative OR subatmospheric) NEAR/3 pressure):ab,ti OR ('vacuum assisted':ab,ti AND adj3:ab,ti AND closure*:ab,ti) OR vac:ab,ti OR 'bandages and dressings'/exp OR bandage*:ab,ti OR dressing*:ab,ti OR 'topical therapy':ab,ti OR 'wound therapy':ab,ti) AND ([dutch]/lim OR [english]/lim) AND [embase]/lim AND [1995-2015]/py (136) – 96 unique |
